Difference between revisions of "Influence of the Text Neck Posture on the Static Dental Occlusion"
| Line 93: | Line 93: | ||
==== Examination Procedure ==== | ==== Examination Procedure ==== | ||
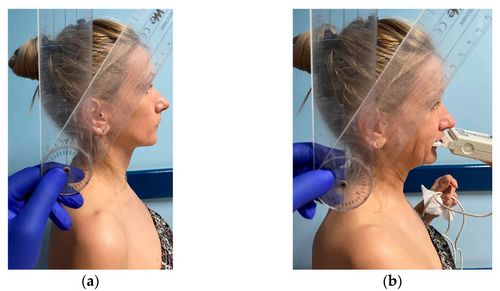
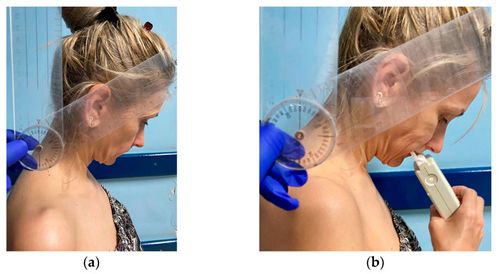
At the beginning of the procedure, we explained the different steps of the examination to our subjects without giving any details about the purpose or hypotheses of the research. The images in Figure 2 and Figure 3 present one of the examiners as she demonstrates the NHP (Figure 2) and the TNP (Figure 3) to the study subjects. | At the beginning of the procedure, we explained the different steps of the examination to our subjects without giving any details about the purpose or hypotheses of the research. The images in Figure 2 and Figure 3 present one of the examiners as she demonstrates the NHP (Figure 2) and the TNP (Figure 3) to the study subjects. | ||
[[File:Stoica 2a.jpeg|center|thumb|500x500px|Figure 2: ('''a''') Measurement of the neck flexion angle with a manual goniometer in NHP; ('''b''') T-Scan registration in NHP.]] | [[File:Stoica 2a.jpeg|center|thumb|500x500px|'''Figure 2:''' ('''a''') Measurement of the neck flexion angle with a manual goniometer in NHP; ('''b''') T-Scan registration in NHP.]] | ||
[[File:Stoica 3.jpeg|center|thumb|500x500px|Figure 3: ('''a''') Measurement of the neck flexion angle with a manual goniometer in TNP; ('''b''') T-Scan registration in TNP.]] | [[File:Stoica 3.jpeg|center|thumb|500x500px|'''Figure 3:''' ('''a''') Measurement of the neck flexion angle with a manual goniometer in TNP; ('''b''') T-Scan registration in TNP.]] | ||
Further on, the subjects were instructed on how to adopt an NHP. Then they were asked to text for 60 s on their mobile phones, in order to relax and get accustomed to the TNP. For most of them, the mandible went into the postural position (with the freeway space between the dental arches) during texting, but each one of them swallowed at some point in MI, which was the position we followed in our research. The data from the dental literature showed a mean spontaneous swallowing frequency of 0.98 swallows/minute for healthy young subjects.<ref>Bulmer J.M., Ewers C., Drinnan M.J., Ewan V.C. Evaluation of spontaneous swallow frequency in healthy people and those with, or at risk of developing, dysphagia: A review. Gerontol. Geriatr. Med. 2021;7:23337214211041801. doi: 10.1177/23337214211041801.</ref> | Further on, the subjects were instructed on how to adopt an NHP. Then they were asked to text for 60 s on their mobile phones, in order to relax and get accustomed to the TNP. For most of them, the mandible went into the postural position (with the freeway space between the dental arches) during texting, but each one of them swallowed at some point in MI, which was the position we followed in our research. The data from the dental literature showed a mean spontaneous swallowing frequency of 0.98 swallows/minute for healthy young subjects.<ref>Bulmer J.M., Ewers C., Drinnan M.J., Ewan V.C. Evaluation of spontaneous swallow frequency in healthy people and those with, or at risk of developing, dysphagia: A review. Gerontol. Geriatr. Med. 2021;7:23337214211041801. doi: 10.1177/23337214211041801.</ref> | ||
| Line 106: | Line 106: | ||
The distribution, force, and timing of occlusal contacts were analyzed in MI and in static intercuspation. The latter was defined by Kerstein as the moment of the last tooth contact during the closure of the mouth, which is marked as the Bline on the registration. It is different from the MI, which appears later.<ref name=":6" /><ref name=":7">Kerstein R.B., Grundset K. Obtaining measurable bilateral simultaneous occlusal contacts with computer-analyzed and guided occlusal adjustments. Quintessence Int. 2001;32:7–18. </ref><ref name=":8">Kerstein R.B. Handbook of Research on Clinical Applications of Computerized Occlusal Analysis in Dental Medicine. 1st ed. IGI Global; Hershey, PA, USA: 2015. T-Scan 8 recording dynamics, system features and clinician user skills; pp. 95–151. </ref> The maximum intercuspation was analyzed in the maximum area frame of the registration (MA). In an ideal occlusion, the MA frame is also the frame where the ''maximum movie force'' (MMF) occurs. | The distribution, force, and timing of occlusal contacts were analyzed in MI and in static intercuspation. The latter was defined by Kerstein as the moment of the last tooth contact during the closure of the mouth, which is marked as the Bline on the registration. It is different from the MI, which appears later.<ref name=":6" /><ref name=":7">Kerstein R.B., Grundset K. Obtaining measurable bilateral simultaneous occlusal contacts with computer-analyzed and guided occlusal adjustments. Quintessence Int. 2001;32:7–18. </ref><ref name=":8">Kerstein R.B. Handbook of Research on Clinical Applications of Computerized Occlusal Analysis in Dental Medicine. 1st ed. IGI Global; Hershey, PA, USA: 2015. T-Scan 8 recording dynamics, system features and clinician user skills; pp. 95–151. </ref> The maximum intercuspation was analyzed in the maximum area frame of the registration (MA). In an ideal occlusion, the MA frame is also the frame where the ''maximum movie force'' (MMF) occurs. | ||
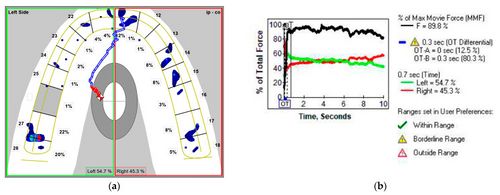
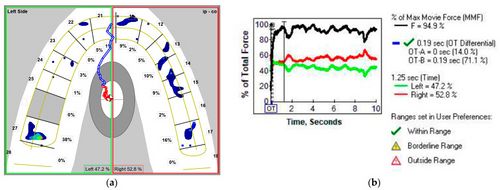
The first analyzed occlusal parameter was ''occlusion time'' (OT)—Figure 4b and Figure 5b—defined by Kerstein as the elapsed time (in seconds) measured from the first occlusal contact (A line) until the last tooth contact in static intercuspation (B line) during mouth closure.<ref name=":7" /><ref name=":8" /> The T-Scan III system was set at a normal OT value of under 0.3 s (“within range”); the “borderline range” was 0.3 to 0.5 s.<ref name=":6" />{{Bib}} | The first analyzed occlusal parameter was ''occlusion time'' (OT)—Figure 4b and Figure 5b—defined by Kerstein as the elapsed time (in seconds) measured from the first occlusal contact (A line) until the last tooth contact in static intercuspation (B line) during mouth closure.<ref name=":7" /><ref name=":8" /> The T-Scan III system was set at a normal OT value of under 0.3 s (“within range”); the “borderline range” was 0.3 to 0.5 s.<ref name=":6" /> | ||
[[File:Stoica 4.jpeg|center|thumb|500x500px|'''Figure 4:''' MA frame of the T-Scan registration of MC subject in NHP: ('''a''') two-dimensional (2D) view with the distribution of the occlusal force between the left and the right side of the arch; ('''b''') graph of the % of the total force in time, with %MMF, OT, OTB, and MAT (0.7 s).]] | |||
[[File:Stoica 5.jpeg|center|thumb|500x500px|'''Figure 5:''' MA frame of the T-Scan registration of MC subject in TNP: ('''a''') 2D view with the distribution of the occlusal force between the left and the right side of the arch; ('''b''') graph of the % of the total force in time, with %MMF, OT, OTB, and MAT (1.25 s).]] | |||
In the MA frame (MI), the following aspects were investigated (Figure 4 and Figure 5): | |||
* (i) ''Distribution of the occlusal force'' between the left and right SSS side of the arch (Figure 4a and Figure 5a). The ideal occlusion has 50% of the occlusal force on each side, but the T-Scan III System Manual states that a distribution of 53% to 47% of the occlusal force can be considered within the normal range.<ref name=":6" /> Based on these values, we ''calculated the asymmetry index of the occlusal force''(AOF) according to the formula:<ref>Wang C., Yin X. Occlusal risk factors associated with temporomandibular disorders in young adults with normal occlusions. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2012;114:419–423. doi: 10.1016/j.oooo.2011.10.039. </ref> '''AOF (%) = [(occlusal force on the right side−occlusal force on the left side)/total occlusal force] × 100''' AOF has normal values ranging from 0 to 6%. | |||
* (ii) ''Percent of the maximum movie force'' (%MMF)—Figure 4b and Figure 5b. In an ideal occlusion, the MA frame is the frame with the largest area of tooth contact, but also the frame with the MMF. | |||
* (iii) ''Time elapsed from the last occlusal contact in static intercuspation till MI'' (MAT-OTB). It describes the time that passes till the slopes of the guiding cusps bring the mandible into MI. This parameter was calculated by subtracting the OTB value from the MAT value. Both values are displayed by the T-Scan software (Figure 4b and Figure 5b). | |||
Statistical processing was performed using the SPSS 17.0 software package. Descriptive statistics were calculated for several continuous variables: OT, AOF, %MMF, and MAT-OTB. The comparisons between the two paired numerical series were performed using the non-parametric Wilcoxon Signed Ranks Test. The results were considered significant for a value of ''p'' < 0.05. The correlations between variable pairs were made by calculating the Spearman’s correlation coefficient, since they did not have a normal distribution. The correlations were considered significant for a value of ''p'' < 0.05, as well. | |||
=== Results === | |||
The demographic characteristics of the study group are presented in Table 1. | |||
{| class="wikitable" | |||
|+ | |||
| | |||
= Table 1 = | |||
Demographic characteristics of the study group. | |||
{| class="wikitable" | |||
! colspan="1" rowspan="1" |Variable | |||
! colspan="2" rowspan="1" |Characteristics | |||
|- | |||
| colspan="1" rowspan="2" |'''Gender—''n'' (%)''' | |||
| colspan="1" rowspan="1" |Male | |||
| colspan="1" rowspan="1" |4 (21.1%) | |||
|- | |||
| colspan="1" rowspan="1" |Female | |||
| colspan="1" rowspan="1" |15 (78.9%) | |||
|- | |||
| colspan="1" rowspan="1" |'''Age''' | |||
| colspan="2" rowspan="1" | | |||
|- | |||
| colspan="1" rowspan="1" |Mean (standard deviation) | |||
| colspan="2" rowspan="1" |21.32 (0.95) | |||
|- | |||
| colspan="1" rowspan="1" |Median (interquartile range) | |||
| colspan="2" rowspan="1" |21.00 (1.00) | |||
|} | |||
|} | |||
The values of the OT were 1.34 ± 1.84 s in NHP and 1.32 ± 1.8 s in TNP, while the difference between the two head and neck positions was small and not statistically significant (''p'' = 0.658), as presented in Table 2. The values of the AOF were 14.88 ± 10.39% in NHP and 18.04 ± 12.83% in TNP; the increase in AOF in TNP was not statistically significant (''p'' = 0.344)—Table 2. The values of the MAT-OTB were 2.08 ± 1.82 s in NHP and 1.45 ± 2.3 s in TNP. Therefore, the decrease in MAT-OTB in TNP was not statistically significant (''p'' = 0.117)—Table 2. The values of the %MMF were 97.5 ± 2.83% in NHP and 96.31 ± 3.17% in TNP; the difference between the two head and neck positions was small and not statistically significant (''p'' = 0.251). The fact that the studied parameters’ variations between the two head and neck positions were not statistically significant could be due to the choice of the NHP as the starting position of our T-Scan study. Adding 30° to the neck flexion angle measured in NHP could have brought the handle and the power cable of the T-Scan into an inappropriate position, leading to the collection of TNP parameter values that were not conclusive in some subjects. | |||
{| class="wikitable" | |||
|+ | |||
| | |||
= Table 2 = | |||
Descriptive statistics and ''p'' values obtained from the applied Wilcoxon Signed Ranks Test. | |||
{| class="wikitable" | |||
! colspan="1" rowspan="1" |Variable | |||
! colspan="1" rowspan="1" |Mean ± Standard Deviation | |||
! colspan="1" rowspan="1" |Median (Interquartile Range) | |||
! colspan="1" rowspan="1" |''p'' 1 | |||
|- | |||
| colspan="1" rowspan="1" |OTN | |||
| colspan="1" rowspan="1" |1.34 ± 1.84 | |||
| colspan="1" rowspan="1" |0.41 (1.22) | |||
| colspan="1" rowspan="2" |0.658 | |||
|- | |||
| colspan="1" rowspan="1" |OT30 | |||
| colspan="1" rowspan="1" |1.32 ± 1.8 | |||
| colspan="1" rowspan="1" |0.45 (1.39) | |||
|- | |||
| colspan="1" rowspan="1" |AOFN | |||
| colspan="1" rowspan="1" |14.88 ± 10.39 | |||
| colspan="1" rowspan="1" |10.8 (21.2) | |||
| colspan="1" rowspan="2" |0.344 | |||
|- | |||
| colspan="1" rowspan="1" |AOF30 | |||
| colspan="1" rowspan="1" |18.04 ± 12.87 | |||
| colspan="1" rowspan="1" |17.1 (16.4) | |||
|- | |||
| colspan="1" rowspan="1" |MMFN | |||
| colspan="1" rowspan="1" |97.5 ± 2.83 | |||
| colspan="1" rowspan="1" |98.3 (2.3) | |||
| colspan="1" rowspan="2" |0.251 | |||
|- | |||
| colspan="1" rowspan="1" |MMF30 | |||
| colspan="1" rowspan="1" |96.31 ± 3.17 | |||
| colspan="1" rowspan="1" |97.7 (4.9) | |||
|- | |||
| colspan="1" rowspan="1" |MAT-OTBN | |||
| colspan="1" rowspan="1" |2.08 ± 1.82 | |||
| colspan="1" rowspan="1" |1.95 (2.76) | |||
| colspan="1" rowspan="2" |0.117 | |||
|- | |||
| colspan="1" rowspan="1" |MAT-OTB30 | |||
| colspan="1" rowspan="1" |1.45 ± 2.3 | |||
| colspan="1" rowspan="1" |0.85 (1.28) | |||
|} | |||
1 Statistically significant ''p'' < 0.05. | |||
|} | |||
Although NHP was inappropriate as a starting point to simulate the TNP in our T-Scan study, the recordings made in that position revealed some significant and useful results. Thus, the mean value of the AOF was 14.88 ± 10.39% in NHP. Perfect symmetry of the occlusal force in MI was not found in any subject, nor in the NHP. Instead, we found an AOF less than or equal to 6% in four subjects with NHP (i.e., subject number 15, 16, 17, and 19; 21.05%). All other subjects had AOF values above 6%, which indicate an unbalanced distribution of the occlusal forces between the right and left side of the dental arches in NHP. The actual distribution of occlusal forces between the left and right side of the arch in each subject can be observed in Supplementary Material Table S1. | |||
The mean value of the OT was 1.34 ± 1.84 s in NHP. Bilateral simultaneous occlusal contacts in static intercuspation are generally associated with an OT under 0.2 s <ref name=":7" /><ref name=":8" /> or 0.3 s.<ref name=":6" /> In NHP, we found an OT below 0.3 s in only four subjects (i.e., subject number 7, 8, 17, and 19; 21.05%). All other subjects had OT values above 0.3 s, which revealed a lack of simultaneity of the occlusal contacts in static intercuspation. The OT values of all subjects can be viewed in Supplementary Material Table S1. | |||
The correlation between OT and AOF was significant, direct, and strong in NHP (Spearman’s rho = 0.724, ''p'' < 0.001)—Figure 6. An increased OT was associated with an increased AOF. The lack of simultaneity of the occlusal contacts in static intercuspation (as concluded from high OT values), associated with an unbalanced distribution of the occlusal forces between the right and left side of the dental arches in MI (high AOF values), point to an unstable static occlusion in NHP. | |||
{{Bib}} | |||
Revision as of 15:01, 10 June 2023
| Title | Influence of the Text Neck Posture on the Static Dental Occlusion |
| Authors | Eniko Tunde Stoica^1 · Corina Marcauteanu · Anca Tudor · Virgil-Florin Duma · Elena Constanta Amaricai · Roxana Onofrei · Oana Suciu · Meda Lavinia Negrutiu · Cosmin Sinescu |
| Source | Document |
| Date | 2022 |
| Journal | Medicina (Kaunas) |
| DOI | 10.3390/medicina58091303 |
| PUBMED | https://pubmed.ncbi.nlm.nih.gov/36143980/ |
| PDF copy | |
| License | CC BY |
| This resource has been identified as a Free Scientific Resource, this is why Masticationpedia presents it here as a mean of gratitude toward the Authors, with appreciation for their choice of releasing it open to anyone's access | |
This is free scientific content. It has been released with a free license, this is why we can present it here now, for your convenience. Free knowledge, free access to scientific knowledge is a right of yours; it helps Science to grow, it helps you to have access to Science
This content was relased with a 'CC BY' license.
You might perhaps wish to thank the Author/s
Free resource by Eniko Tunde Stoica^1 · Corina Marcauteanu · Anca Tudor · Virgil-Florin Duma · Elena Constanta Amaricai · Roxana Onofrei · Oana Suciu · Meda Lavinia Negrutiu · Cosmin Sinescu
|
TADERP Research Center, “Victor Babes” University of Medicine and Pharmacy of Timisoara, 9 Revolutiei 1989 Ave., 300070 Timisoara, Romania; moc.oohay@najmedokine
2School of Dental Medicine, “Victor Babes” University of Medicine and Pharmacy of Timisoara, 2A Eftimie Murgu Place, 300070 Timisoara, Romania; or.tfmu@roduta (A.T.); moc.oohay@uiturgen_adem (M.L.N.); moc.liamg@ucsenisonim (C.S.)
3Research Center in Dental Medicine Using Conventional and Alternative Technologies, School of Dental Medicine, “Victor Babes” University of Medicine and Pharmacy of Timisoara, 9 Revolutiei 1989 Ave., 300070 Timisoara, Romania; or.tfmu@anele.iacirama
43OM Optomechatronics Group, Faculty of Engineering, “Aurel Vlaicu” University of Arad, 2 Elena Dragoi Str., 310177 Arad, Romania
5Doctoral School, Polytechnic University of Timisoara, 1 Mihai Viteazu Ave., 300222 Timisoara, Romania
6Department of Rehabilitation, Physical Medicine and Rheumatology, Research Center for Assessment of Human Motion, Functionality and Disability, “Victor Babes” University of Medicine and Pharmacy of Timisoara, 2A Eftimie Murgu Place, 300070 Timisoara, Romania; or.tfmu@anaxor.ierfono (R.O.); or.tfmu@87uicusanao (O.S.)
*Correspondence: moc.oohay@iroc_acram (C.M.); gro.rebmemaso@ligriv.amud (V.-F.D.); Tel.: +40-741-182-478 (C.M.); +40-751-511-451 (V.-F.D.)
Abstract
Background and Objectives: The excessive use of smartphones for various tasks led to a new adverse postural phenomenon called text neck. The aim of this study was to investigate the effect of the text neck posture (TNP) on static occlusion by using the T-Scan III occlusal diagnostic system. Materials and Methods: Nineteen subjects (aged 20 to 24 years) were considered for this research. They had normal values for anterior overbite and overjet, Angle Class I occlusion, no posterior crossbite, and no signs or symptoms of cervical or temporo-mandibular disorders. Occlusal registrations were performed with the T-Scan III system in a normal, neutral head posture (NHP), as well as in the TNP. The investigated parameters were: occlusion time (OT), asymmetry index of the occlusal force (AOF), percent of the maximum movie force (%MMF), and the time elapsed from the last occlusal contact until the maximum intercuspation (MAT-OTB). The last three parameters were analyzed in the maximum area frame (MA) of the registrations. For the statistical analysis of the recorded data, the Wilcoxon Signed Ranks test and the Spearman’s correlation coefficient were used. Results: The following values were obtained in NHP and in TNP: for AOF, 14.88 ± 10.39% and 18.04 ± 12.83%, respectively; for OT, 1.34 ± 1.84 s and 1.32 ± 1.8 s, respectively; for the %MMF, 97.5 ± 2.83% and 96.31 ± 3.17%, respectively; for MAT-OTB, 2.08 ± 1.82 s and 1.45 ± 2.3 s, respectively. There were no statistically significant differences between the static occlusal parameters measured in NHP and those in TNP. However, the high values of the AOF and OT in NHP revealed an imbalance of the occlusal force distribution between the right and left side in maximum intercuspation (MI), as well as a lack of simultaneity of static occlusal contacts. Furthermore, there was a significant, direct, and strong correlation between OT and AOF in NHP. Conclusions: The NHP should not be used as the starting position in TNP simulations in T-Scan studies, so as to avoid statistically insignificant differences between static occlusion in NHP and TNP. The healthy standing subjects, with normal occlusal relationships from the clinical point of view, revealed an occlusal instability in NHP when examined with the T-Scan.
Keywords: text neck posture (TNP), static occlusion, maximum intercuspation (MI), T-Scan III system, occlusion time (OT), asymmetry index of the occlusal force (AOF)
Introduction
The term text neck was proposed by a chiropractor, Dr. Dean L. Fishman,[1] and it is used to define both a bad postural position and a syndrome associated with the prolonged and inappropriate use of handheld mobile devices, including smartphones.[2][3][4] This adverse postural phenomenon can be described as a sustained flexed neck position, with the head tilted forward. It is associated with forward-rolled shoulders, which increase the curve of the thoracic spine. [2][4] Compared to the neutral posture, the higher neck flexion angle requires an increased activity of the neck muscles in order to compensate for the effect of gravity.[5] These biomechanical changes in the cervical and thoracic spine, as well as muscular imbalances and postural compensations, finally lead to cervical muscle fatigue and pain. [2][3]
The scientific literature demonstrates that any change in the head and neck posture induces a change in the rest position of the mandible,[6] in the activity of the masticatory muscles,[7] and in the habitual path of mouth closing.[8] In an interesting study, Yamada et al. (1999) found that as the head bended forward (i.e., in ventroflexion), the closing path approached the maximum intercuspation position (MIP) from the anterior region.[9] The forward bending of the head also decreased the stability of the closing path. On the other hand, as the head was bent backward, the closing path approached the MIP from the posterior region and its stability increased.
A widely debated topic in the literature is whether or not changes in head and neck posture have a significant influence on dental occlusion. However, the effect of text neck posture (TNP) on occlusion has been overlooked in the dental literature. Chapman et al. (1991) used the T-Scan system to record and analyze the occlusal contacts that occur in maximum intercuspation (MI) in three different head positions: supine, sitting erect, and sitting with the head tipped forward.[10] They proved that the mandible is pushed forward during closure when the head is tipped forward, resulting in more anterior initial contacts. However, the total number of occlusal contacts in MI was not significantly modified by the postural change. This means that the main effect of a changed head position was on the initial tooth contacts, which guide the mandible back into MI from eccentric positions. The authors speculated that the location of the first occlusal contacts in the anterior region of the dental arches during closure (i.e., when the head is tipped forward) could produce occlusal overload of the individual teeth. Therefore, they are expected to alter the activity of the elevator muscles.
In another T-Scan study of mouth closure, Makofsky et al. (1991) found that in subjects 30 years of age and older, a 30° ventroflexion of the head shifted the initial occlusal contacts anteriorly, while a 45° head extension displaced the contacts posteriorly older.[11] Gupta et al. (2017) reported that the occlusal contact area in MI varies between two different head postures: 90° upright and 30° ventroflexed [12].[12] The pressed occlusal contact area (mm2) was measured using the Dental Prescale System (Dental Prescale, Fuji Film Co., Tokyo, Japan), a computerized occlusal analysis system used for the measurement and analysis of the bite force (N), the occlusal contact area (mm2), and the bite pressure (MPa). They concluded that the pressed occlusal contact area (mm2) decreased in head ventroflexion compared to the upright-erect position.
Such studies have proved that physiological head positions, which are adopted naturally by the subjects, have a significant influence on some of the investigated static occlusal parameters, including the number and position of the initial tooth contacts during mouth closure, as well as on the occlusal contact area in MI. It must be pointed out that a 30° ventroflexion of the head coincides with the active feeding posture, while a 45° head extension is used for drinking.[13]
Fewer studies have addressed the effect of abnormal head positions such as the forward head posture(FHP) on dental occlusion. In FHP, the subject pushes her/his head in front of its natural position over the cervical spine, with a simultaneous posterior bending of the head and a compensatory extension of the upper cervical spine, in order to maintain the horizontal direction of the eyes—for example, facing the computer desktop[14] (Figure 1a). Some authors even call this the desktop neck posture.[15]
In a sample of thirty-nine normal subjects, Makofsky (2000) did not find a significant relationship between experimentally induced FHP and the initial occlusal contact pattern that occured while the subject was slowly and completely biting onto the sensor of the T-Scan II Occlusal Diagnostic System.[16] This result is of interest because the same author proved in a previous study that the initial occlusal contact pattern during closure is influenced by the extension of the head.[11] It appears that in FHP, which involves a significant degree of head and upper cervical spine extension, the alteration in the mandibular position is not important enough to produce the occlusal changes observed during a physiological head extension. This conclusion has clinical relevance in the treatment of patients with temporo-mandibular disorders (TMD) and FHP. Some authors claim a relationship between FHP and TMD.[17][18] If the initial occlusal contact pattern does not change in FHP, that means that the occlusion is not an etiological factor of the TMD and should not be therapeutically addressed.
It must be pointed out that FHP is different from the TNP (as pointed out in Figure 1), although they are often incorrectly used as synonyms. Assumed while using a smartphone, the TNP is characterized by a flexed position of the upper cervical region, with the eyes facing downward and fixed on the smartphone[2]—Figure 1b.
Following the impact of this aspect on today’s population, as well as the shortcomings of the literature on this topic, as pointed out above, the aim of this study was to investigate the influence of TNP on static occlusion in young healthy subjects with normal occlusal relationships.
Materials and Methods
The present study was conducted according to the guidelines of the Declaration of Helsinki. It was approved by CECS no. 70/22.12.2021 of the Ethical Committee of the “Victor Babes” University of Medicine and Pharmacy of Timisoara, Romania.
Study Subjects
A total of nineteen subjects, fifteen females and four males (aged 20 to 24 years), were considered for this research. This sample was chosen for convenience. The process of consecutive selection among young subjects who were interested in a free examination of their masticatory system was based on the following inclusion criteria: full dental arches (except for the third molars in some subjects); normal values of overbite (2 to 4 mm) and overjet (1 to 2 mm); Angle Class I occlusion, without posterior crossbite; healthy periodontal status, with normal physiological tooth mobility; no signs and symptoms of TMD; no pain or limited range of motion in the cervical spine.
In addition, all standing subjects were able to adopt a normal head posture (NHP), with the head and back straight and with the external auditory meatus on the same vertical line as the acromio-clavicular joint (i.e., the shoulder), the hip, and the knee. Their head was placed in the midline, with the chin above the manubrium, while their neck had a slight lordotic curve and a normal length, without tilting or rotation of the head.[19]
The exclusion criteria were: degenerative or inflammatory spine pathology; fibro-myalgia; cervical spine traumatic events; autoimmune diseases; and neurologic diseases that can have an impact on cervical position. Furthermore, we excluded subjects that currently reported any of the following parafunctions, which can influence the head and neck position by muscle hyperactivity: awake and/or sleep bruxism; nail biting; biting of the cheeks and lips; ventral position during sleep; keeping the phone between the face and the shoulder; playing violin or a wind instrument; maintaining a pencil between the dental arches; tongue pressing on the lingual surfaces of teeth; abusive consumption of chewing gum.[20]
The anamnesis and clinical examination of the masticatory system was based on Schiffman’s “Diagnostic Criteria for Temporomandibular Disorders (DC/TMD) for Clinical and Research Applications”.[21] The examination of the cervical area was based on the protocol recommended by Ombregt.[19]
All subjects were fully informed about the nature of the investigation and signed an informed consent form to participate in this research.
Examination Procedure
At the beginning of the procedure, we explained the different steps of the examination to our subjects without giving any details about the purpose or hypotheses of the research. The images in Figure 2 and Figure 3 present one of the examiners as she demonstrates the NHP (Figure 2) and the TNP (Figure 3) to the study subjects.
Further on, the subjects were instructed on how to adopt an NHP. Then they were asked to text for 60 s on their mobile phones, in order to relax and get accustomed to the TNP. For most of them, the mandible went into the postural position (with the freeway space between the dental arches) during texting, but each one of them swallowed at some point in MI, which was the position we followed in our research. The data from the dental literature showed a mean spontaneous swallowing frequency of 0.98 swallows/minute for healthy young subjects.[22]
Each occlusion was objectively assessed by the same examiner by using the T-Scan III system (Tekscan Inc., Ann Arbor, MI, USA), following a standardized protocol. Thus, the standing subject was asked to hold the scanning handle and to adopt an NHP, with the head and back straight and with the external auditory meatus on the same vertical line as the acromio-clavicular joint (i.e., the shoulder), the hip, and the knee. A second examiner measured the neck flexion angle of the subject in NHP with a manual goniometer. This neck flexion angle is defined as the angle between a vertical line raised from the C7 spinous process and a line connecting the C7 spinous process to the mid-tragus.[5] The subject was instructed to forcefully clench on the sensor while the T-Scan occlusal registration was made. No pain was elicited in the masticatory system or in the cervical area. In the following phase, each subject was asked to further flex his neck forward, till she/he reached a neck flexion angle that was 30° higher than the angle measured in NHP. A new T-Scan registration was made in this TNP.
The digital occlusal analysis of each patient was preceded by mock registrations that allowed the patient to get accustomed to the procedure. At the same time, we could adjust the sensitivity of the T-Scan III system in order to ensure that its force recording range was matched to the “bite strength” of each individual patient.[23] We changed the sensor before taking the actual recordings.
The T-Scan III movies were saved and labeled in a way that blinded the data collectors who analyzed those movies. Thus, they did not know in which head and neck position each of the recordings was made.
Data Collection and Statistical Analysis
The distribution, force, and timing of occlusal contacts were analyzed in MI and in static intercuspation. The latter was defined by Kerstein as the moment of the last tooth contact during the closure of the mouth, which is marked as the Bline on the registration. It is different from the MI, which appears later.[23][24][25] The maximum intercuspation was analyzed in the maximum area frame of the registration (MA). In an ideal occlusion, the MA frame is also the frame where the maximum movie force (MMF) occurs.
The first analyzed occlusal parameter was occlusion time (OT)—Figure 4b and Figure 5b—defined by Kerstein as the elapsed time (in seconds) measured from the first occlusal contact (A line) until the last tooth contact in static intercuspation (B line) during mouth closure.[24][25] The T-Scan III system was set at a normal OT value of under 0.3 s (“within range”); the “borderline range” was 0.3 to 0.5 s.[23]
In the MA frame (MI), the following aspects were investigated (Figure 4 and Figure 5):
- (i) Distribution of the occlusal force between the left and right SSS side of the arch (Figure 4a and Figure 5a). The ideal occlusion has 50% of the occlusal force on each side, but the T-Scan III System Manual states that a distribution of 53% to 47% of the occlusal force can be considered within the normal range.[23] Based on these values, we calculated the asymmetry index of the occlusal force(AOF) according to the formula:[26] AOF (%) = [(occlusal force on the right side−occlusal force on the left side)/total occlusal force] × 100 AOF has normal values ranging from 0 to 6%.
- (ii) Percent of the maximum movie force (%MMF)—Figure 4b and Figure 5b. In an ideal occlusion, the MA frame is the frame with the largest area of tooth contact, but also the frame with the MMF.
- (iii) Time elapsed from the last occlusal contact in static intercuspation till MI (MAT-OTB). It describes the time that passes till the slopes of the guiding cusps bring the mandible into MI. This parameter was calculated by subtracting the OTB value from the MAT value. Both values are displayed by the T-Scan software (Figure 4b and Figure 5b).
Statistical processing was performed using the SPSS 17.0 software package. Descriptive statistics were calculated for several continuous variables: OT, AOF, %MMF, and MAT-OTB. The comparisons between the two paired numerical series were performed using the non-parametric Wilcoxon Signed Ranks Test. The results were considered significant for a value of p < 0.05. The correlations between variable pairs were made by calculating the Spearman’s correlation coefficient, since they did not have a normal distribution. The correlations were considered significant for a value of p < 0.05, as well.
Results
The demographic characteristics of the study group are presented in Table 1.
Table 1Demographic characteristics of the study group.
| |||||||||||||||||
The values of the OT were 1.34 ± 1.84 s in NHP and 1.32 ± 1.8 s in TNP, while the difference between the two head and neck positions was small and not statistically significant (p = 0.658), as presented in Table 2. The values of the AOF were 14.88 ± 10.39% in NHP and 18.04 ± 12.83% in TNP; the increase in AOF in TNP was not statistically significant (p = 0.344)—Table 2. The values of the MAT-OTB were 2.08 ± 1.82 s in NHP and 1.45 ± 2.3 s in TNP. Therefore, the decrease in MAT-OTB in TNP was not statistically significant (p = 0.117)—Table 2. The values of the %MMF were 97.5 ± 2.83% in NHP and 96.31 ± 3.17% in TNP; the difference between the two head and neck positions was small and not statistically significant (p = 0.251). The fact that the studied parameters’ variations between the two head and neck positions were not statistically significant could be due to the choice of the NHP as the starting position of our T-Scan study. Adding 30° to the neck flexion angle measured in NHP could have brought the handle and the power cable of the T-Scan into an inappropriate position, leading to the collection of TNP parameter values that were not conclusive in some subjects.
Table 2Descriptive statistics and p values obtained from the applied Wilcoxon Signed Ranks Test.
1 Statistically significant p < 0.05. |
Although NHP was inappropriate as a starting point to simulate the TNP in our T-Scan study, the recordings made in that position revealed some significant and useful results. Thus, the mean value of the AOF was 14.88 ± 10.39% in NHP. Perfect symmetry of the occlusal force in MI was not found in any subject, nor in the NHP. Instead, we found an AOF less than or equal to 6% in four subjects with NHP (i.e., subject number 15, 16, 17, and 19; 21.05%). All other subjects had AOF values above 6%, which indicate an unbalanced distribution of the occlusal forces between the right and left side of the dental arches in NHP. The actual distribution of occlusal forces between the left and right side of the arch in each subject can be observed in Supplementary Material Table S1.
The mean value of the OT was 1.34 ± 1.84 s in NHP. Bilateral simultaneous occlusal contacts in static intercuspation are generally associated with an OT under 0.2 s [24][25] or 0.3 s.[23] In NHP, we found an OT below 0.3 s in only four subjects (i.e., subject number 7, 8, 17, and 19; 21.05%). All other subjects had OT values above 0.3 s, which revealed a lack of simultaneity of the occlusal contacts in static intercuspation. The OT values of all subjects can be viewed in Supplementary Material Table S1.
The correlation between OT and AOF was significant, direct, and strong in NHP (Spearman’s rho = 0.724, p < 0.001)—Figure 6. An increased OT was associated with an increased AOF. The lack of simultaneity of the occlusal contacts in static intercuspation (as concluded from high OT values), associated with an unbalanced distribution of the occlusal forces between the right and left side of the dental arches in MI (high AOF values), point to an unstable static occlusion in NHP.
- ↑ Neupane S., Ali U.I., Mathew A. Text neck syndrome-systematic review. Imp. J. Interdiscip. Res. 2017;3:141–148. [Google Scholar] [Ref list]
- ↑ 2.0 2.1 2.2 2.3 Fiebert I., Kistner F., Gissendanner C., DaSilva C. Text neck: An adverse postural phenomenon. Work. 2021;69:1261–1270. doi: 10.3233/WOR-213547.
- ↑ 3.0 3.1 Cuéllar J.M., Lanman T.H. “Text neck”: An epidemic of the modern era of cell phones? Spine J. 2017;17:901–902. doi: 10.1016/j.spinee.2017.03.009.
- ↑ 4.0 4.1 Moreno M.A., Hoopes A.J. Technology and Adolescent Health: In Schools and Beyond.Academic Press; Cambridge, MA, USA: 2020. The impact of digital media; p. 367.
- ↑ 5.0 5.1 Ailneni R.C., Syamala K.R., Kim I.S., Hwang J. Influence of the wearable posture correction sensor on head and neck posture: Sitting and standing workstations. Work. 2019;62:27–35. doi: 10.3233/WOR-182839
- ↑ Darling D.W., Kraus S., Glasheen-Wray M.B. Relationship of head posture and the rest position of the mandible. J. Prosthet. Dentistry. 1984;52:111–115. doi: 10.1016/0022-3913(84)90192-6
- ↑ Boyd C.H., Slagle W.F., Boyd C.M., Bryant R.W., Wiygul J.P. The effect of head position on electromyographic evaluations of representative mandibular positioning muscle groups. CRANIO® 1987;5:50–54. doi: 10.1080/08869634.1987.11678174.
- ↑ Goldstein D.F., Kraus S.L., Willams W.B., Glasheen-Wray M. Influence of cervical posture on mandibular movement. J. Prosthet. Dent. 1984;52:421–426. doi: 10.1016/0022-3913(84)90460-8.
- ↑ Yamada R., Ogawa T., Koyano K. The effect of head posture on direction and stability of mandibular closing movement. J. Oral Rehabil. 1999;26:511–520. doi: 10.1046/j.1365-2842.1999.00386.x.
- ↑ Chapman R.J., Maness W.L., Osorio J. Occlusal contact variation with changes in head position. Int. J. Prosthodont. 1991;4:377–381.
- ↑ 11.0 11.1 Makofsky H.W., Sexton T.R., Diamond D.Z., Sexton M.T. The effect of head posture on muscle contact position using the T-Scan system of occlusal analysis. CRANIO® 1991;9:316–321. doi: 10.1080/08869634.1991.11678378.
- ↑ Gupta S., Tarannum F., Gupta N.K., Upadhyay M., Abdullah A. Effect of head posture on tooth contacts in dentate and complete denture wearers using computerized occlusal analysis system. J. Indian Prosthodont. Soc. 2017;17:250–254. doi: 10.4103/jips.jips_321_16.
- ↑ Haralur S.B., Al-Gadhaan S.M., Al-Qahtani A.S., Mossa A., Al-Shehri W.A., Addas M.K. Influence of functional head postures on the dynamic functional occlusal parameters. Ann. Med. Health Sci. Res. 2014;4:562–566. doi: 10.4103/2141-9248.139319.
- ↑ Patwardhan A.G., Khayatzadeh S., Havey R.M., Voronov L.I., Smith Z.A., Kalmanson O., Ghanayem A.J., Sears W. Cervical sagittal balance: A biomechanical perspective can help clinical practice. Eur. Spine J. 2018;27:25–38. doi: 10.1007/s00586-017-5367-1.
- ↑ (accessed on 20 July 2022)]. Available online: https://erikdalton.com/blog/text-neck-desktop-neck [Ref list]
- ↑ Makofsky H.W. The influence of forward head posture on dental occlusion. CRANIO® 2000;18:30–39. doi: 10.1080/08869634.2000.11746111.
- ↑ Lee W.Y., Okeson J.P., Lindroth J. The relationship between forward head posture and temporomandibular disorders. J. Orofac. Pain. 1995;9:161–167.
- ↑ Huggare J.A., Raustia A.M., Makofsky H.W. Head posture and cervicovertebral and craniofacial morphology in patients with craniomandibular dysfunction. CRANIO® 1992;10:173–179. doi: 10.1080/08869634.1992.11677908.
- ↑ 19.0 19.1 Ombregt L. A system of Orthopaedic Medicine. 3rd ed. Churchill Livingstone Elsevier; London, UK: 2013. Clinical Evaluation of the cervical spine; pp. 119–133.
- ↑ Okeson J.P. Management of Temporo-Mandibular Disorders and Occlusion. 7th ed. The Mosby Imprint of Elsevier Inc.; St. Louis, MI, USA: 2013. Etiology of functional disturbances in the masticatory system; pp. 102–128.
- ↑ Schiffman E., Ohrbach R. Executive summary of the Diagnostic Criteria for Temporomandibular Disorders for clinical and research applications. J. Am. Dent. Assoc. 2016;147:438–445. doi: 10.1016/j.adaj.2016.01.007.
- ↑ Bulmer J.M., Ewers C., Drinnan M.J., Ewan V.C. Evaluation of spontaneous swallow frequency in healthy people and those with, or at risk of developing, dysphagia: A review. Gerontol. Geriatr. Med. 2021;7:23337214211041801. doi: 10.1177/23337214211041801.
- ↑ 23.0 23.1 23.2 23.3 23.4 T-Scan III Manual. [(accessed on 1 July 2022)]. Available online: https://archive.org/details/manualzilla-id-5684279[Ref list]
- ↑ 24.0 24.1 24.2 Kerstein R.B., Grundset K. Obtaining measurable bilateral simultaneous occlusal contacts with computer-analyzed and guided occlusal adjustments. Quintessence Int. 2001;32:7–18.
- ↑ 25.0 25.1 25.2 Kerstein R.B. Handbook of Research on Clinical Applications of Computerized Occlusal Analysis in Dental Medicine. 1st ed. IGI Global; Hershey, PA, USA: 2015. T-Scan 8 recording dynamics, system features and clinician user skills; pp. 95–151.
- ↑ Wang C., Yin X. Occlusal risk factors associated with temporomandibular disorders in young adults with normal occlusions. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2012;114:419–423. doi: 10.1016/j.oooo.2011.10.039.